
The real risk in senior medication isn’t just forgetfulness; it’s the hidden dangers of complex regimens and a fragmented healthcare system that simple tools can’t solve.
- Standard pillboxes create a “filled pillbox illusion,” giving a false sense of security without confirming a dose was actually taken.
- The risk of harmful drug interactions and adverse effects increases dramatically once a person is taking five or more different medications.
Recommendation: Shift from passive reminders to an active monitoring system, and proactively request a structured medication review (SMR) from your GP or local pharmacist to de-prescribe unnecessary drugs.
For any carer in the UK supporting a senior loved one, the colourful 7-day pill organiser is a familiar sight. It represents order, control, and a simple solution to a complex problem. We fill it diligently every Sunday, believing we’ve secured another week of medication safety. But what if this sense of security is an illusion? When the daily medication list grows to eight, nine, or more different pills—for blood pressure, diabetes, arthritis, and more—this basic tool begins to fail, often silently and with dangerous consequences.
The common advice is to set more reminders or to be more organised. However, the root of the problem isn’t just memory. It’s the overwhelming cognitive load of managing multiple dosing times, specific instructions (e.g., “with food”), and potential interactions. Research shows that almost 50% of older adults struggle with managing their medications, a challenge that escalates with every new prescription added by a different NHS specialist. As one expert notes, the core issues are polypharmacy and memory, creating a complex web that a simple plastic box cannot untangle.
But if the standard pillbox is a failing system, what is the alternative? The answer lies not in simply buying a more expensive gadget, but in understanding *when* and *why* an upgrade is necessary. This involves moving from a passive organisation tool to an active monitoring framework. This guide will provide a clinical-based approach for carers to assess the true risks in their loved one’s regimen, decide when to transition to smarter technology, and, most importantly, address the systemic issue of fragmented care that often causes the medication overload in the first place.
This article provides a comprehensive framework to help you navigate these challenges. Below, you will find detailed sections covering the critical failure points of manual systems, a guide to programming advanced dispensers, and strategies for working within the NHS to ensure genuine patient safety.
Summary: A Carer’s Guide to Advanced Medication Management
- Why Does a 7-Day Pill Organiser Stop Working When You Take 8 Different Medications?
- How to Programme an Automatic Pill Dispenser to Prevent Both Missed and Double Doses?
- Simple Alarmed Pillbox vs Wi-Fi Connected Dispenser: Which Is Worth the Extra £200?
- The Filled Pillbox Illusion: How to Know If Your Relative Actually Takes Their Medications
- When Should You Upgrade from Manual Pillbox to Automatic Dispenser Based on Error Frequency?
- The 8-Medication Threshold Where Drug Interactions Start Causing More Harm Than Benefit
- How to Configure Alexa or Google Home to Call for Help, Control Lights, and Set Medication Reminders?
- Why Does Every NHS Specialist Treat One Condition While Your Overall Health Declines?
Why Does a 7-Day Pill Organiser Stop Working When You Take 8 Different Medications?
A standard 7-day pillbox works on a simple, trust-based premise: if a compartment is empty, the medication was taken. This system is effective for one or two daily pills. However, once the regimen expands to eight or more medications—a state known as polypharmacy—the cognitive load required to manage them correctly exceeds the capacity of both the user and the tool. The challenge is no longer just remembering to take a pill; it’s managing a complex matrix of timings, dosages, and specific instructions, a task that can overwhelm even the most diligent individual.
This breakdown occurs due to what specialists call cognitive load saturation. Each new medication adds variables: Does it need to be taken with food? Can it be taken with the others? What about the half-pill dose? This mental juggling act leads to errors not of forgetfulness, but of confusion. As Dr. Ceppie Merry, a medical expert, explains in a guide to senior medication management:
The two key challenges that seniors face are polypharmacy (taking lots of pills) and remembering to take them. It can be really complex to remember what to take and when to take them.
– Dr. Ceppie Merry, SingleCare medication management guide
The pillbox, with its uniform compartments, offers no way to manage this complexity. It cannot alert for a missed dose, prevent a double dose if the user is confused, or account for medications with variable schedules. It becomes a passive container rather than an active safety tool, creating a dangerous false sense of security for carers. The system fails because it was designed for simplicity, but the reality of modern geriatric medicine is anything but.

This visual of an unstable, cascading tower of pill bottles perfectly symbolizes the mental burden. Each bottle represents a medication, and the precarious balance shows how adding just one more can lead to the collapse of the entire system. This is precisely what happens when a simple pillbox is tasked with a job it was never designed for: managing the high-stakes complexity of polypharmacy.
How to Programme an Automatic Pill Dispenser to Prevent Both Missed and Double Doses?
Transitioning to an automatic pill dispenser is a significant step towards enhancing medication safety, but its effectiveness hinges entirely on meticulous and accurate programming. Unlike a simple pillbox, these devices are active systems designed to lock away future doses and dispense only the correct pills at the correct time. This prevents both common errors: a senior forgetting a dose, or a confused individual taking a second dose because they forgot the first. The goal is to create a foolproof system, and that requires a rigorous setup protocol.
Case Study: Reducing Errors in a Care Setting
A nursing home that implemented a voice-activated automatic pill dispenser system provides a powerful example. The facility reported a measurable decrease in medication errors and a significant increase in patient satisfaction. By providing both audio and visual alerts, the system ensured residents received their medications at the correct times, all while reducing the burden on nursing staff for manual distribution. This demonstrates that when programmed correctly, these devices are a powerful intervention.
Achieving this level of success requires treating the dispenser not as a simple gadget, but as a piece of medical equipment. The programming must be flawless, as a single mistake can replicate itself daily until the next refill. Below is a critical audit plan to ensure your automatic dispenser is a reliable safety net, not another source of risk.
Action Plan: Your Dispenser Setup and Audit Protocol
- Medication Reconciliation: Before touching the device, conduct a mandatory audit with a pharmacist. Bring all pill bottles and prescriptions to create a single, undisputed “source of truth” for the current medication schedule. This is the most critical step.
- System Configuration: Based on the pharmacist-verified schedule, choose the correct daily dosage ring for the dispenser (e.g., 4 times a day). Correctly load the pills into the tray, ensuring you never place medication in any red-flagged or locked-out sections.
- Programming the Schedule: Carefully set the current time on the device. Then, meticulously program each alarm time to match the reconciled schedule. Double-check AM/PM settings and adjust alarm tones and volumes for the user’s hearing ability.
- Full System Test Run: Before loading the actual medications, conduct a complete 24-hour test run using harmless items like small sweets or vitamins. Verify that the device rotates, alarms, and dispenses at exactly the right times.
- Contingency and Security: Create a written plan for what to do in case of a power cut or device malfunction. Once the system is tested and loaded with real medication, close and lock the cover to prevent tampering or accidental overdoses.
Simple Alarmed Pillbox vs Wi-Fi Connected Dispenser: Which Is Worth the Extra £200?
The decision to upgrade from a basic pillbox often leads to a choice between two main categories of technology: a simple alarmed pillbox (costing around £50) and a sophisticated, Wi-Fi connected automatic dispenser (often £200-£300 plus potential subscription fees). The significant price difference can be a barrier, but framing the decision solely on cost is a mistake. The real question is one of risk management. The higher cost buys an entirely different level of safety and monitoring, which can be priceless.
The stakes are incredibly high. In the UK and US, medication errors are a leading cause of preventable harm in older adults. While specific UK data is compiled differently, safety data from the US indicates that between 7,000 and 9,000 people die annually from medication errors. Investing in a system that actively prevents these errors is an investment in a loved one’s health and longevity. The choice is not about saving £200; it’s about choosing the right level of protection for a specific set of risks.
To make an informed decision, a feature-by-feature comparison is essential. The following table breaks down the capabilities of each device type, helping you align the features with the specific needs and risks of the person you are caring for. Please note that costs are illustrative and may vary based on the model and supplier in the UK.
| Feature | Simple Alarmed Pillbox | Wi-Fi Connected Dispenser |
|---|---|---|
| Initial Cost | £40-£70 | £200-£300 (plus potential subscription fees) |
| Medication Capacity | 28 compartments (weekly doses) | Up to 60 cups (10+ days, multiple doses) |
| Alert System | Sound and light alarms only | Sound, light, plus smartphone notifications to caregivers |
| Adherence Tracking | None (visual inspection required) | Automatic digital logs accessible remotely |
| Caregiver Monitoring | Requires in-person check or phone calls | Real-time alerts and adherence reports via app |
| Programming Complexity | Simple manual setup (6 daily alarms max) | Initial setup may require professional or family assistance |
| Power Dependency | Battery-operated (low failure risk) | Requires electrical outlet and Wi-Fi (vulnerable to outages) |
| Best For | Simple forgetfulness, single senior household | Complex regimens, high-risk medications, remote caregiver oversight |
The Wi-Fi connected dispenser is the clear choice for individuals with complex regimens, cognitive impairment, or high-risk medications. Its ability to provide remote monitoring and alerts to a carer’s smartphone transforms medication management from a passive, hope-based system to an active, data-driven one. This is the key feature that justifies the additional cost.
The Filled Pillbox Illusion: How to Know If Your Relative Actually Takes Their Medications
One of the most dangerous aspects of relying on a standard pillbox is what I call the “filled pillbox illusion.” A carer arrives, sees the compartments for Monday and Tuesday are empty, and breathes a sigh of relief. The assumption is that the medication was taken. However, this provides no actual proof of adherence. The pills could have been dropped, thrown away, or simply forgotten on a side table. Without active monitoring, you are operating with adherence data-blindness, a state of not knowing what is really happening.
Detecting non-adherence requires a more investigative approach, looking for proxy indicators—indirect signs that medication is not being taken as prescribed. This means shifting focus from the pillbox itself to the person and their health outcomes. Researchers have found that some patients, particularly the elderly, may choose to stop taking medication if they feel better or are bothered by side effects. As one study on geriatric patients notes:
Geriatric patients especially have a tendency to stop taking drugs off their own when they consider their symptoms have been ameliorated. This can hinder the expected improvement in adherence.
– Researchers at tertiary care hospital study, PMC study on medication compliance in geriatric patients
To see through the illusion, carers must become detectives. Here are several practical methods for detecting potential non-adherence, even when the pillbox appears to be used correctly:
- Track Core Health Metrics: The medication is prescribed to achieve a result. Monitor what it’s meant to control. If blood pressure readings are creeping up, blood sugar levels are unstable, or pain is worsening despite an “empty” pillbox, it is a major red flag.
- Correlate Symptoms with Timings: Document when symptoms worsen. For example, if pain medication should be providing relief in the afternoon but the person consistently reports high pain levels at that time, the dose may have been missed.
- Conduct Discreet Pill Counts: Periodically and discreetly count the remaining pills in the original pharmacy bottles. Compare the count to the expected usage based on the prescription date. A surplus of pills is a clear sign of missed doses.
- Monitor Prescription Refill Patterns: Keep an eye on when repeat prescriptions are requested from the GP or pharmacy. If a 30-day supply is lasting 40 days, doses are being missed. Conversely, requesting refills too early could signal double-dosing.
- Listen for Clues of Intentional Non-Adherence: Pay attention to comments like “This pill makes me dizzy,” “I don’t think I need it anymore,” or “I feel fine without it.” These statements often signal a deliberate choice to stop taking medication.
When Should You Upgrade from Manual Pillbox to Automatic Dispenser Based on Error Frequency?
The decision to upgrade from a manual pillbox to an automatic dispenser shouldn’t be a gut feeling. It should be a clinical decision based on a clear-eyed assessment of risk. Not all medication errors are equal. Forgetting a vitamin is a low-risk event; missing a dose of a blood thinner or insulin can be a medical emergency. Therefore, the trigger for upgrading should be based on the severity of the error, not just the frequency.
This is especially critical for the large number of older adults with cognitive challenges. With studies indicating that approximately 40 percent of older adults live with memory impairment, relying on a system that requires perfect memory is inherently flawed. A single, critical error is a far more compelling reason to upgrade than frequent, low-impact mistakes. The goal is to intervene before a catastrophic error occurs, not after.
To help carers and families make this crucial decision, here is an error severity framework. Use this checklist to determine your “upgrade trigger point.”
- Severity Level 1 (Monitor): A Missed Vitamin or Supplement. If the user occasionally misses non-critical pills with no immediate health impact, you can continue with the manual system but increase oversight and reminders.
- Severity Level 2 (Plan Upgrade): One Missed Maintenance Medication. If a dose of a maintenance drug like a statin or blood pressure pill is missed even once a month, it’s a sign the current system is failing. Begin researching automatic options immediately.
- Severity Level 3 (Upgrade Immediately): Any Missed Critical Medication. If a single dose of a high-risk medication is missed—including blood thinners (e.g., Warfarin), insulin, seizure medication, or cardiac drugs—an upgrade is non-negotiable and should be implemented within the week.
- The “Near Miss” Indicator (Upgrade Same Day): The moment a carer catches themselves almost putting the wrong pill in a compartment, or a senior almost takes their morning pills in the evening, the manual system has proven to be unsafe. This is a critical failure warning; upgrade immediately.
- The Frequency Override Rule: Even if errors are infrequent, if the user asks “Did I take my pills?” more than once a week, or if there is any diagnosed cognitive decline, the system is no longer appropriate. An automatic dispenser with tracking is essential, regardless of error history. The same applies if they struggle with vision to read labels or dexterity to open bottles.
This framework shifts the focus from counting mistakes to weighing their potential consequences. A single checkmark in Level 3 is a definitive signal that the manual system’s risks have become unacceptable.
The 8-Medication Threshold Where Drug Interactions Start Causing More Harm Than Benefit
While this article’s title mentions eight medications as a tipping point for organisational failure, the clinical danger zone for polypharmacy begins much earlier. From a pharmacological safety perspective, the risks of adverse drug reactions (ADRs) and negative interactions start to increase exponentially once a patient is on five or more medications. According to the National Center for Biotechnology Information, polypharmacy is clinically defined as the routine use of 5 or more medications. By the time a regimen reaches eight drugs, the potential for harm is substantial.
The danger of polypharmacy is insidious because its symptoms are often mistaken for signs of old age. A loved one might seem more tired, confused, or unsteady on their feet. The family and even doctors might attribute this to the natural aging process, when in fact it could be the direct result of a drug interaction or a side effect. This masking effect is one of the greatest challenges in geriatric medicine.
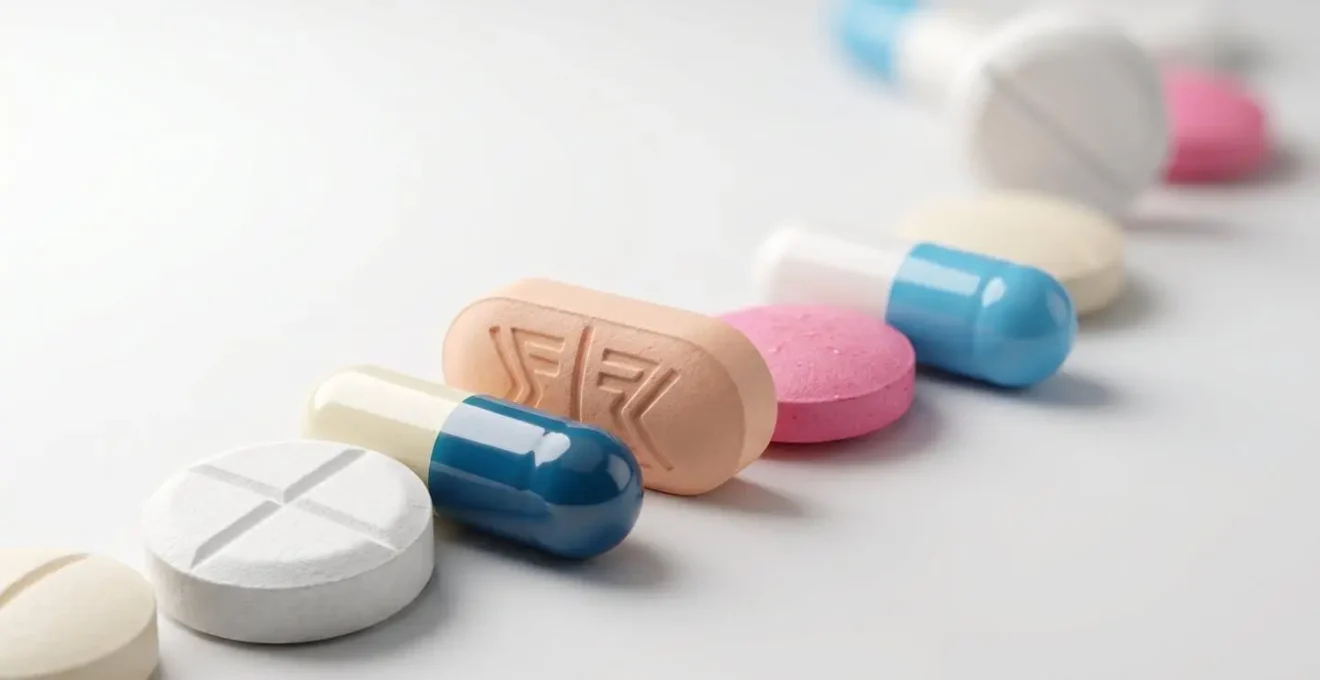
This domino-like cascade of pills perfectly illustrates the problem. One medication causes a side effect (e.g., dizziness), which is then treated with another medication, which in turn causes another side effect (e.g., dry mouth), and so on. As the National Center for Biotechnology Information warns:
Polypharmacy can be overlooked because of the symptoms it causes as a result of drug interactions or side effects of drugs, for example, tiredness, sleepiness, decreased alertness, constipation, diarrhea, incontinence, loss of appetite, confusion, falls, depression, or lack of interest in usual activities, may be confused with symptoms of normal aging.
– National Center for Biotechnology Information, StatPearls – Polypharmacy
Therefore, any senior on five or more medications should be considered at high risk. The focus must shift from simply managing the logistics of pill-taking to actively questioning the necessity of every single drug on the list. A comprehensive medication review with a GP or clinical pharmacist is not just good practice; it is an essential safety intervention to dismantle the “prescribing cascade” before it causes irreversible harm.
How to Configure Alexa or Google Home to Call for Help, Control Lights, and Set Medication Reminders?
While dedicated automatic pill dispensers are the gold standard for high-risk patients, existing smart home technology like Amazon Alexa or Google Home can be configured to create a powerful, low-cost adherence and safety system. For seniors who are comfortable with voice commands, these devices can offer more than simple reminders; they can create a multi-layered system of alerts, confirmations, and even escalations to a caregiver. This transforms a passive speaker into an active participant in a loved one’s care plan.
Case Study: Voice Reminders Improve Adherence
A study involving seniors using Amazon Alexa for medication reminders found a marked improvement in adherence rates. Participants felt more in control of their schedules and valued the system’s ease of use. The voice-activated interface was particularly effective for those with limited tech experience or visual impairments, demonstrating that familiar technology can be successfully repurposed for health management.
The key is to move beyond a single alarm and build a “Routine” with an escalation path. This means the system doesn’t just announce the reminder; it checks for a response and takes further action if one isn’t given. Here is a step-by-step guide to configuring a robust medication routine using the Alexa app:
- Create a “Medication Time” Routine: In the Alexa app, go to Routines and create a new routine. Set the trigger to be a specific time (e.g., “8:00 AM”).
- Add Multi-Modal Alerts: For the routine’s action, add several layers of alerts. First, an announcement like, “It’s time for your morning medication.” Second, if you have smart lights, program them to flash a specific colour (e.g., green). Third, play a distinct sound or chime.
- Set Up Verbal Confirmation: The crucial next step is to program Alexa to listen for a confirmation phrase, such as “Alexa, I’ve taken my medication.” This tells the system the task is complete.
- Configure an Escalation Sequence: If no confirmation is heard within 10 minutes, the routine should trigger a second, more insistent alert (e.g., a louder alarm and a spoken warning like, “Your 8:00 AM medication has not been confirmed.”).
- Program a Caregiver Notification: If there is still no confirmation after 15 minutes, the system must escalate externally. Using services like Alexa’s Emergency Assist or an integration tool (IFTTT), configure the routine to automatically send a text message or place a call to a designated caregiver’s phone.
- Set Up the Emergency Feature: Separately, ensure the “Call for help” feature is configured. This allows the user to say “Alexa, call for help” to contact a designated emergency contact. It is vital to understand that in the UK, Alexa cannot call 999 directly; a separate medical alert system is still recommended for emergencies.
Key Takeaways
- The transition from a simple pillbox to an automated system should be driven by an “error severity framework,” not just error frequency. One critical mistake outweighs many minor ones.
- True medication adherence can only be verified through active monitoring systems or by tracking health outcomes, not by looking at an empty pillbox.
- Anyone taking five or more medications is at risk of polypharmacy and requires a proactive medication review with their GP or a clinical pharmacist to challenge the necessity of every drug.
Why Does Every NHS Specialist Treat One Condition While Your Overall Health Declines?
The problem of polypharmacy and medication overload doesn’t start in the home; it often begins in the fragmented structure of our healthcare system. An older adult in the UK might see a cardiologist for their heart, an endocrinologist for their diabetes, and a rheumatologist for their arthritis. Each NHS specialist, acting with the best intentions, prescribes medication to manage the specific condition they are treating. The result is an ever-growing list of drugs, with no single clinician having a holistic view of the patient’s total medication burden.
This siloed approach is the primary driver of the “prescribing cascade.” As experts at Johns Hopkins Medicine explain, this occurs when a new drug is prescribed to treat the side effects of another drug, creating a domino effect. For instance, a blood pressure medication might cause swollen ankles, leading to a prescription for a diuretic, which might then cause dehydration or electrolyte imbalance, leading to yet another prescription. The problem is compounded by the staggering number of unnecessary medications people take. Alarming studies indicate that over 50% of older adults are taking at least one medication that is not clinically indicated.
This is a systemic failure, and it cannot be solved with a better pillbox alone. The ultimate solution lies in proactive medication stewardship. As a carer or patient, you have the right to challenge this fragmentation. The most powerful tool at your disposal is to request a Structured Medication Review (SMR) with your GP or a clinical pharmacist. This is a comprehensive, holistic review of all medications—including prescriptions, over-the-counter drugs, and supplements—with the explicit goal of “de-prescribing,” or safely stopping, any drugs that are unnecessary, ineffective, or causing harm.
Prescription cascade can occur when patients are prescribed medications to offset side effects caused by other drugs they are taking, compounding the risk of polypharmacy.
– Johns Hopkins Medicine, Polypharmacy in Adults 60 and Older
Tackling polypharmacy requires a fundamental shift in perspective. Instead of just asking “How can we manage all these pills?”, we must start asking, “Does my loved one really need to be on all these pills?”. Pushing for this conversation within the NHS is the most critical step you can take to ensure long-term health and safety, moving beyond simply managing chaos to actively reducing it.
The journey from a simple pillbox to a comprehensive safety strategy requires diligence, awareness, and advocacy. By assessing risk, choosing the right technology, and demanding integrated care from the NHS, you can move beyond the illusion of safety and build a genuine system of support. The next logical step is to book a structured medication review with your GP or pharmacist to put this knowledge into action.